Clinical trials serve as a tool to discover new treatments and detect and diagnose diseases. Their importance cannot be underestimated. Unfortunately, as important as these clinical trials are, there is an area of the trials that are lacking, which may be risking public health.
According to research from the Centers for Disease Control and Prevention, racial and ethnic minority populations experience higher rates of poor health and disease in a range of health conditions, when compared to their Caucasian counterparts.
These health conditions include diabetes, hypertension, obesity, asthma, and heart disease. What’s more, the fact that the life expectancy among Black/African Americans is four years lower than that of White Americans. Despite these facts, racial and ethnic minority populations are still extremely underrepresented in clinical trials.
Clinical trials provide answers that can protect public health. However, are these answers really protecting our longevity, or are they widening health disparities and inequities even further?
The lack of diversity in clinical trials is a threat to public health
“The U.S. population has become increasingly diverse, and ensuring meaningful representation of racial and ethnic minorities in clinical trials for regulated medical products is fundamental to public health.
Going forward, achieving greater diversity will be a key focus throughout the FDA to facilitate the development of better treatments and better ways to fight diseases that often disproportionately impact diverse communities.” – Robert M. Califf, M.D., FDA Commissioner
According to a study published in JAMA Network Open that analyzed data from completed interventional vaccine trials between July 2011 and June 2020, only 43% of the trials reported data on race or ethnicity. What’s more, white individuals were found to be (over) represented 77.9% of the time in clinical trials. This number is shocking, especially when the researchers noted how the other races and ethnicities were represented:
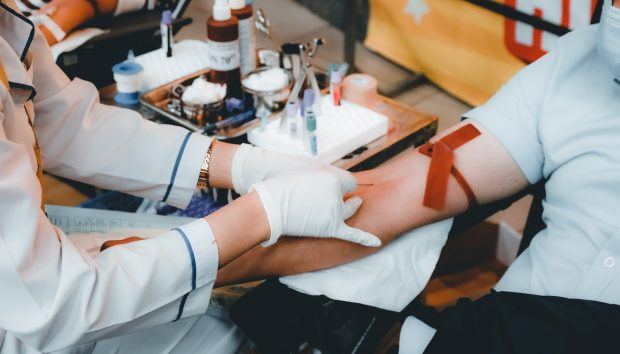
Photo by Nguyễn Hiệp on Unsplash
- Hispanic or Latino participants were represented just 11.6% of the time.
- Black or African American participants were represented only 10.6% of the time.
- Asian and American Indian participants were represented 5.7% of the time.
- Alaska Native participants were represented 0.4 percent of the time.
If that’s not enough, the researchers also noted the following:
- 48.5% of the trials did not include American Indian or Alaska Native participants
- 60.4% did not include Hawaiian or Pacific Islander participants
Why diversity matters in medical research
We all have different racial, ethnic, and socio-economic backgrounds. As such, diseases, treatment options, and therapies are not going to affect us in the same manner. A diverse population in clinical trials can produce data on how a treatment or disease operates. This then allows for researchers to make better-informed decisions about public health.
For instance, while black women and white women develop breast cancer at similar rates, black women are 40% more likely to die from the disease. Yet, research has found that black women are significantly underrepresented in breast cancer trials. The lack of diversity in breast cancer trials means that the medicines and therapies being tested and approved may not necessarily be effective in a group that is most impacted by the disease.
“We need everyone appropriately represented because we want to make sure a therapy works the same way and the side effects are the same in different populations. We also want to make sure we are providing precision medicine.
Sometimes a medicine might work better in one population than another. We need to learn these things up front so we can give each patient the right medicine at the right time.” –Dr. Karen Winkfield, MD, PhD, radiation oncologist told BreastCancer.Org
Why is there a lack of diversity in clinical trials?
1. Not finding out about clinical trial opportunities
One of the biggest obstacles to the lack of diversity in clinical trials is the fact that the wider population isn’t aware of any clinical trial opportunities.
Either their doctors are unaware of ongoing clinical trials, or they may have an unconscious bias that convinces them that people of color have no desire or interest to partake in clinical trials. Unfortunately, without a doctor’s support, you wouldn’t get far when if you’re looking for information on any up-and-coming clinical trials.
2. Strict eligibility criteria
Eligibility criteria are guidelines that clinical trials have, and they are essentially a checklist that one has to adhere to if they’re hoping to be eligible to join the clinical trial. These guidelines are set so that researchers can confirm that the study results are not influenced by external factors.

Photo by National Cancer Institute on Unsplash
The guidelines also help protect participants. While factors such as age and gender are understandable, other criteria may be too strict, such as high blood pressure or diabetes, and this can prevent people from being eligible to join.
3. Heavy expenses
While clinical trials generally cover the costs of anything related to the trial, participants are still expected to cover their personal expenses, which include travel and lodging, which can be costly.
4. Lack of trust in the healthcare system
In 2017, Serena Williams experienced health complications while giving birth to her daughter via Cesarean section. When she alerted the nurses to her symptoms, she was continuously ignored until eventually her doctor listened to her and ordered a CT scan. The scan revealed blood clots in her lungs, but following emergency surgery, the clots were successfully removed, and her life was saved.
The harrowing experience that the tennis legend faced wasn’t a unique one, as many women have been in similar situations, especially women of color. According to a 2021 study, black and Hispanic women are less likely than white women to receive endometrial cancer treatment that adheres to medical guidelines.
The discrimination faced by people of color in medical spaces has led to a general mistrust in the healthcare system, which may explain why people of color chose to opt-out of participating in clinical trials.
Improving diverse access to clinical trials
As diversity in clinical trials is important for public health, various health bodies are doing their part to help to encourage this diversity.
Earlier this year, the U.S. Food & Drug Administration (FDA) issued a new draft guideline. The guidelines recommend that sponsors develop a Race and Ethnicity Diversity Plan. The plan will involve the enrollment of adequate numbers of participants in clinical trials from underrepresented racial and ethnic populations in the United States.

Photo by JESHOOTS.COM on Unsplash
Additionally, in June of this year, Johnson & Johnson formed a $5 million sponsorship with Stand Up To Cancer in an effort to boost diversity in early-phase clinical trials. The new deal hopes to address cancer disparities. It hopes to do thus by creating a sustainable, scalable, and replicable approach to removing barriers to Phase 1 and Phase 2 cancer clinical trial participation.
As great as it is that these health bodies are doing their part to address the lack of diversity, frontline workers can also do their part. Improving communication between people of color and healthcare professionals, which also involves said healthcare workers acknowledging how race can influence healthcare, can help to address the lack of diversity in clinical trials.
Bottom line
The success of clinical trials can improve and protect public health. However, this is only if the trials are a true representation of a country’s population. People of color may face hurdles when it comes to joining clinical trials. As such, it is imperative to diversify clinical trials so that the health of everyone is improved and protected.
References
Awidi, M., & Al Hadidi, S. (2021). Participation of Black Americans in Cancer Clinical Trials: Current Challenges and Proposed Solutions. JCO oncology practice, 17(5), 265–271. https://doi.org/10.1200/OP.21.00001
Flores, L. E., Frontera, W. R., Andrasik, M. P., Del Rio, C., Mondríguez-González, A., Price, S. A., Krantz, E. M., Pergam, S. A., & Silver, J. K. (2021). Assessment of the Inclusion of Racial/Ethnic Minority, Female, and Older Individuals in Vaccine Clinical Trials. JAMA network open, 4(2), e2037640. https://doi.org/10.1001/jamanetworkopen.2020.37640
Kaspers, M., Llamocca, E., Quick, A., Dholakia, J., Salani, R., & Felix, A. S. (2020). Black and Hispanic women are less likely than white women to receive guideline-concordant endometrial cancer treatment. American journal of obstetrics and gynecology, 223(3), 398.e1–398.e18. https://doi.org/10.1016/j.ajog.2020.02.041



![women [longevity live]](https://longevitylive.com/wp-content/uploads/2020/01/photo-of-women-walking-down-the-street-1116984-100x100.jpg)













