According to Dr. Ian Chapple, former Head of the School of Dentistry at Birmingham University and speaker at this year’s American Association for the Advancement of Science event, it is unlikely that there is any condition in the body where the microbiome isn’t involved.
With such a strong background in oral health, Dr. Chapple understands that the mouth is a breeding ground for bacteria, so much so that Dr. Chapple has been seeking a link between gum disease and rheumatoid arthritis. Furthermore, additional research has also suggested that poor oral health may even raise the risk for Alzheimer’s disease.
The Link Between Mouth Bacteria and Chronic Diseases
Rheumatoid arthritis
It all comes down to inflammation
Rheumatoid arthritis is an inflammatory condition whereby the immune system begins attacking the body’s joints.
Speaking of inflammation, it’s also the root cause of many dental diseases. As both RA and dental diseases have inflammation in common, there has been a consensus that the two are linked.
Certain bacteria in your mouth can trigger inflammation and cause dental diseases. The thinking is that this bacteria may also trigger the onset of RA.
What does the research say?
According to a 2008 German study published in the Journal of Periodontology. participants who had RA faced 8 times the risk of developing gum disease as compared with people without RA.
A 2013 study from the University of Louisville in Kentucky found that the bacterium that causes periodontal disease, Porphyromonas gingivalis, not only increases the severity of rheumatoid arthritis, but it can also leads to an earlier onset of the disease as well as cause a quicker progression of symptoms.
A 2015 study from Johns Hopkins Arthritis Center found that out of 100 RA patients, 70% of them had at least moderate gum disease.
A later meta-analysis from 2016 that examined 21 studies on the topic found that the dental diseases periodontitis was 13% more common in RA patients than in a control group of people who did not have the disease.
Additionally, a separate study from the same year identified the common bacterium between gum disease and in many people with RA as Aggregatibacter actinomycetemcomitans. According to the researchers, the bacterium causes the overproduction of citrullinated proteins. These proteins have been linked to triggering the development of RA.
So what does this mean?
“The connection can be confusing,”Terrance Griffin, DMD, chair of the department of periodontology at the Tufts University School of Dental Medicine in Boston, told Everyday Health. “There are so many factors that can come into play, like oral hygiene. RA can cause you to lose some dexterity, which may mean you can’t clean your teeth as well. But that may only partially account for this relationship.”
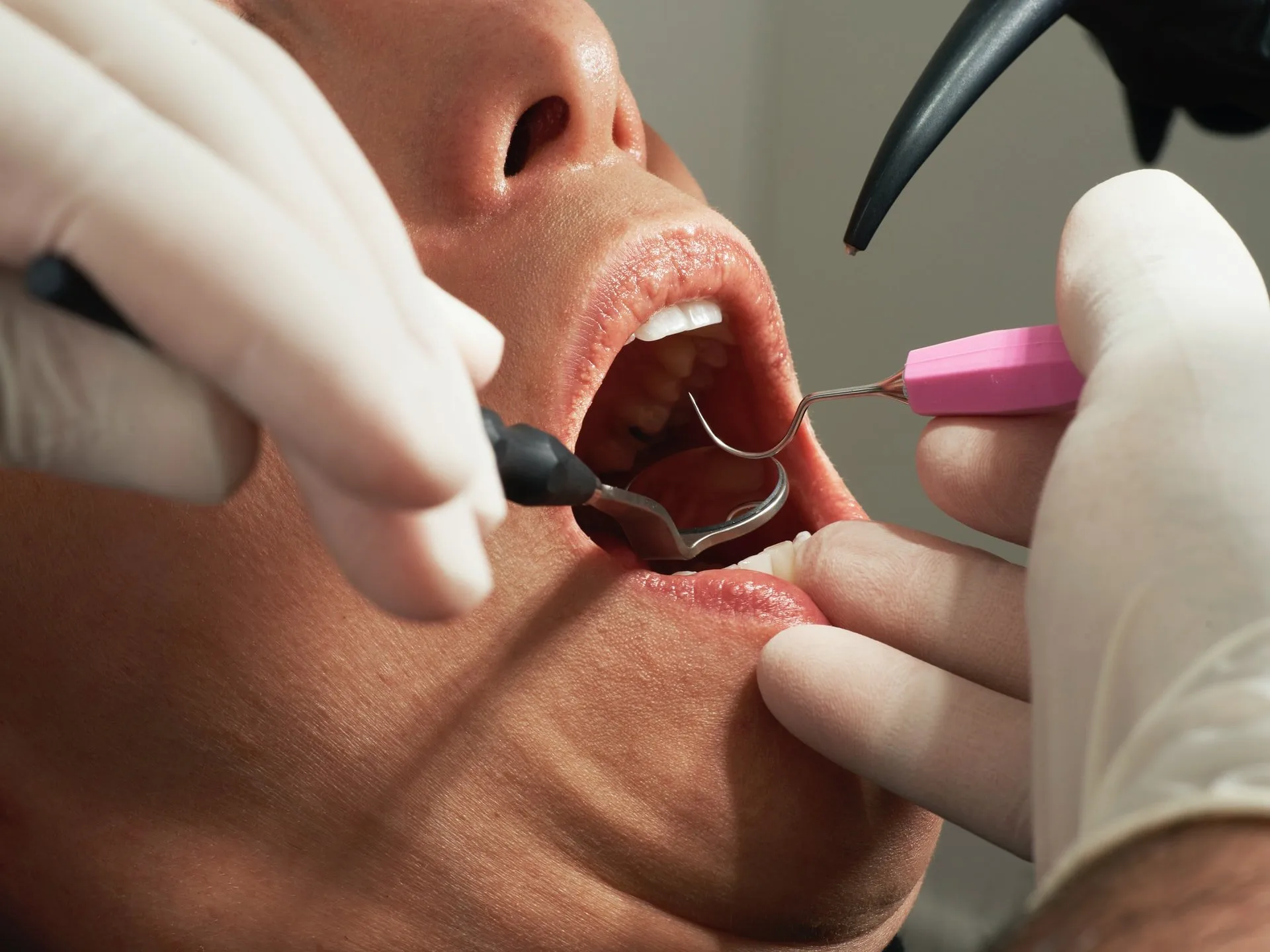
Photo by Caroline LM on Unsplash
Manage Both Conditions By Treating One
According to a small study, individuals with RA who properly managed their oral health noticed an improvement in arthritis pain and symptoms (1).
“People who have both gum disease and RA should have an informed care team comprised of both a physician and a periodontist,” explained Dr. Griffin. “Brushing and flossing can be challenging for those with RA, and you should work with your doctors to find out what works best for you. And if you don’t have a periodontist, get an evaluation from your dentist every year to monitor the status of your gums, since you are more likely to get it.”
What about Alzheimer’s?
Around 50 million people worldwide have Alzheimer’s disease. It appears that poor dental health may increase your risk of becoming a statistic.
Lightspring/Shutterstock
Mouth-brain connection
A 2019 study published in Science Advances suggested the bacteria that causes gingivitis may also be connected to Alzheimer’s disease.
Previous research has found that this species of bacteria, Porphyromonas gingivalis, can move from the mouth to the brain. Once in the brain, the bacteria release enzymes called gingipains. This enzyme can destroy nerve cells, thus increasing the risk for Alzheimer’s.
The aim of the 2019 study was to find evidence of this process in human brains. The researchers examined the brains of 53 deceased people who had been diagnosed with Alzheimer’s. They found high levels of gingipain in almost all of them – 96% to be exact.
“Periodontists have long known that a healthy mouth contributes to a healthy body, and research has suggested an association between periodontal disease and dementia conditions, such as Alzheimer’s,” Dr. Richard Kao, DDS, Ph.D., and president of the American Academy of Periodontology (AAP) said in a statement, “These recent findings present strong evidence on how periodontal disease can impact the pathogenesis of Alzheimer’s disease and should highlight how crucial it is to manage periodontal disease, especially in older adults or individuals who have increased risk for dementia.”
Dental health matters
Here are some tips to keep your teeth happy and healthy.
- Visit a dentist regularly
- Brush twice a day
- Change your toothbrush every 3 months
- Use toothpaste that contains fluoride
- Don’t forget to (gently) floss
- Please don’t smoke

Want to know more?
The lockdown has seen many people practice less healthy lifestyles. This has had a detrimental effect on our dental health. In fact, there are a few hidden dental dangers of lockdown that you may not know about.





![women [longevity live]](https://longevitylive.com/wp-content/uploads/2020/01/photo-of-women-walking-down-the-street-1116984-100x100.jpg)













