Globally, there are over 55 million people living with Alzheimer’s disease, and this figure is projected to hit 78 million by 2030 and 139 million by 2050. With global deaths from Alzheimer’s disease and other dementias nearly tripling over the past 30 years, there’s been an added incentive to find a cure to adequately address this crisis.
Unfortunately, there is currently no cure for Alzheimer’s. However, a new drug promises hope as on July 7, lecanemab received approval from the Food and Drug Administration (FDA) to treat Alzheimer’s disease.
Lecanemab Provides Hope For Alzheimer’s Disease
“Alzheimer’s disease immeasurably incapacitates the lives of those who suffer from it and has devastating effects on their loved ones. This treatment option is the latest therapy to target and affect the underlying disease process of Alzheimer’s, instead of only treating the symptoms of the disease.” – Dr. Billy Dunn, director of the Office of Neuroscience in the FDA’s Center for Drug Evaluation and Research
Lecanemab, which will be sold under the brand name Leqembi, was developed by pharmaceutical companies Eisai and Biogen. Created as a monoclonal antibody, lecanemab attacks and targets Aβ deposits, which are the biggest precursors to the development of Alzheimer’s disease.
“We know that it clears the beta-amyloid plaque,” Dr. Scott A. Kaiser, a geriatrician and director of geriatric cognitive health for the Pacific Neuroscience Institute at Providence Saint John’s Health Center in Santa Monica, CA, told Healthline in September.
“The question is whether or not that actually helps with brain function. But the idea is that these plaques are interfering with the effective communication and overall interaction between brain cells and that clearing them could have positive effects.”
What does the research say?
A study published in the New England Journal of Medicine shared the full findings of Eisai’s Phase 3 Clarity AD clinical trial for lecanemab’s efficacy in slowing the clinical progression of Alzheimer’s.
The trial featured 1795 adults, aged 50 to 90, who suffered from early Alzheimer’s. Half of them received either lecanemab or a placebo.
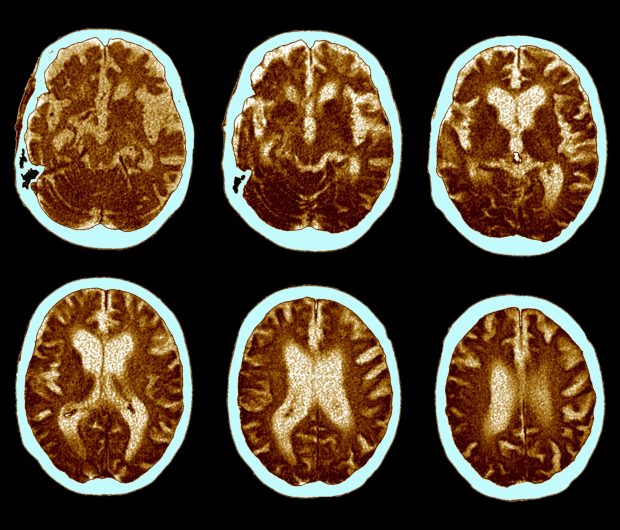
Science Photo Library – ZEPHYR./Getty Images
Per the findings, participants who took lecanemab slowed down their cognitive decline by 27% compared to those who took the placebo. Participants were also 31% less likely to advance to the next stage of Alzheimer’s during the study.
Is it safe?
While the FDA’s approval is a great step towards managing the Alzheimer’s crisis, drugs that target amyloid deposits do come with side effects, and lecanemab is not exempt from this.
14% of patients who took lecanemab experienced micro bleeding in the brain. Also, 12.6% of patients who took lecanemab experienced mild swelling in the brain. That said, Dr. Emer MacSweeney, principal investigator of the trial, said that these abnormalities were asymptomatic (were not felt by patients) and were detected by MRI.
Not everyone supports lecanemab
Howard Fillit, MD, Co-Founder and Chief Science Officer of the Alzheimer’s Drug Discovery Foundation, welcomed the FDA’s decision. Fillit believes that the approval of Leqembi will serve as a catalyst for driving further developments and investments in the Alzheimer’s pipeline.
However, not everyone shares these sentiments.
For one, Dr. Michael Greicius, a professor of neurology and neurological sciences at Stanford University in California, shared with Healthline that the earlier phase 2 trials of lecanemab were flawed. This is because the high dose versus placebo analysis (that showed some clinical benefit) was compromised.
Dr. Greicius added that participants who were carriers of APOE4 (the Alzheimer’s gene) were prevented midway through the trial from receiving a high dose of the treatment. As a result, the trial then had many more APOE4 carriers in the placebo group (71%) than in the high-dose group (30%),
“This difference in percentage of APOE4 carriers is as likely (or in my view more likely) than the drug to account for the difference in clinical outcomes,” Greicius explained.
Another concern is the possibility that many will view lecanemab as an Alzheimer’s cure, and that’s not the case. Joy Snider, a professor of neurology at Washington University School of Medicine, reminds us that lecanemab is neither a cure nor does it make people get better. Rather, it slows down the progression of very mild disease.
How much is it?
Eisai officials SHARED that the fee for the drug will be $26,500 per year for biweekly dosing. This is definitely a hefty fee, with many wondering if the drug’s effectiveness was worth its high price.
That said, the Centers for Medicare and Medicaid Services announced they will provide significant coverage for Leqembi,
“With FDA’s decision, CMS will cover this medication broadly while continuing to gather data that will help us understand how the drug works. This is welcome news for the millions of people in this country and their families who are affected by this debilitating disease.” CMS Administrator Chiquita Brooks-LaSure said in a statement.
The CMS said that people with the original Medicare plan will pay 20% coinsurance of the Medicare-approved amount after meeting their Part B deductible.
Is Alzheimer’s disease coming to an end?
Granted, the FDA’s latest approval is a great weapon in the fight against Alzheimer’s. Yet, this does not mean that the neurodegenerative disease is a thing of the past.
As of this point, we can only wait to see the outcome of the FDA’s approval of lecanemab. That said, we can do our part by adopting lifestyle changes that can slow, as well as prevent, cognitive decline.
So, where to start? Well, one study revealed 7 habits that can help to reduce the risk for cognitive decline.
MAIN IMAGE CREDIT: PopTika/Shuttertsock
References
Li, X., Feng, X., Sun, X., Hou, N., Han, F., & Liu, Y. (2022). Global, regional, and national burden of Alzheimer’s disease and other dementias, 1990–2019. Frontiers in Aging Neuroscience, 14, 937486. https://doi.org/10.3389/fnagi.2022.937486
van Dyck, C. H., Swanson, C. J., Aisen, P., Bateman, R. J., Chen, C., Gee, M., Kanekiyo, M., Li, D., Reyderman, L., Cohen, S., Froelich, L., Katayama, S., Sabbagh, M., Vellas, B., Watson, D., Dhadda, S., Irizarry, M., Kramer, L. D., & Iwatsubo, T. (2022). Lecanemab in Early Alzheimer’s Disease. The New England journal of medicine, 10.1056/NEJMoa2212948. Advance online publication. https://doi.org/10.1056/NEJMoa2212948



![women [longevity live]](https://longevitylive.com/wp-content/uploads/2020/01/photo-of-women-walking-down-the-street-1116984-100x100.jpg)













