MS is a particularly tricky disease to diagnose. Not only are there many potential MS symptoms to consider, but the symptoms can be subtle and mimic that of other ailments, such as depression, other autoimmune diseases, and vitamin deficiencies.
Fortunately, with more MS awareness, including the recent reveal by Selma Blair of her MS diagnosis, people are becoming more and more familiar with this incurable, yet often manageable disease.
By sharing my MS journey, and specifically how I was diagnosed as a medical student, I hope to continue to provide MS awareness.
I also want to encourage those who are experiencing potential MS symptoms to remain persistent in seeking out answers. If you do have MS, the sooner you can begin treatment, the better chance you have of slowing down your disease progression.
My Journey to MS Diagnosis
My multiple sclerosis (MS) journey began somewhat abruptly during my second year of medical school. I was twenty-three years old—thriving, hopeful, and embracing life with a zest and dedication towards my future that seemed unbreakable.
While my days were filled with typically grueling, tedious hours reading and working in the anatomy lab, I relished studying the human body and all its intricacies. Little did I know that at the same time, a neurological disease was wreaking havoc on my body—one that would challenge me for years to come.
Symptom #1: Fatigue
Crushing fatigue hit me first. One sunny fall morning, I simply could not get out of bed. My body was wrapped in heavy steel plates, and my brain felt fuzzy and devoid of thought or emotion.
My first thought was that I had the “flu”. Yet, I had no fever, no muscle aches, and no cold symptoms. I was perplexed, but ultimately figured something was awry, and that I needed to listen to my body and give it some rest.
Despite two days of lying in bed, I experienced zero relief. I may have felt more exhausted if that was even possible. I knew, regardless of how fatigued I was though, I had to get back to school as I had a pressing workload to attend to and anatomy lab partners who needed me.
I forced myself to go to school, trying to ease my fatigue with coffee, healthy snacks, and sheer willpower. The “dragging” of myself throughout each day continued for nearly two weeks – a blurry yet palpable time of suffering.
Symptom #2: Headaches
As the fatigue continued, a new symptom developed—severe, pulsating headaches. It was these headaches that finally prompted me to make an appointment with my primary care doctor.
My doctor diagnosed me with migraines and sent me home with a prescription for pain medication. He also included information on stress management and adhering to a migraine-friendly diet.
Unfortunately, though, for the next few weeks between Thanksgiving and winter break, I continued to endure “off and on” again migraines and persistent fatigue. I managed, somehow, to take my winter exams, suppressing the looming, omnipresent dread that something was “off” with my body.
Symptom #3: Blurry Vision
Although relieved that exams were over and winter break was in effect, I soon began experiencing disturbing eye symptoms—left eye pain and blurry vision. In addition, I felt off balance and was experiencing fleeting numbness and tingling in my legs.
I called my primary care doctor again who referred me to an ophthalmologist (an eye specialist) and a neurologist. Both specialists examined me and reported that I was healthy and had nothing to worry about. No blood or imaging tests were ordered.
I was stunned. I still couldn’t see well. My left eyeball ached, my migraine seemed to never go away, and I was so unbelievably fatigued. Nothing made sense.
The next day, I called my primary care doctor and tearfully relayed my relentless fatigue, migraines, and confusing eye symptoms. She suggested that I may be clinically depressed.
Yes, I thought, I was “depressed.” I am young and vibrant and yet sick, and no one can help me. My doctor prescribed me an anti-depressant, and I begrudgingly filled it.
A Brain MRI: The Key to My MS Diagnosis
I felt lost and completely defeated at this point. I traveled home to the suburbs of Chicago to stay with my parents. Busy with the daily grind of managing my fatigue and studying, coupled with the desire to not worry my parents, I had not disclosed the last several weeks of symptoms in full effect to them.
Upon coming home, my father, a physician, immediately sensed something was not right. His daughter never lay in bed like this. It was my father – how fortunate and rare it is to have a parent in the medical field – who ordered an MRI that would be the key to unlocking my MS diagnosis.
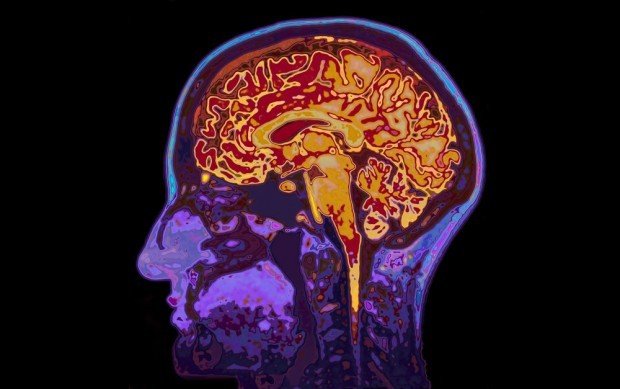
During my brain MRI, I had various characteristic MS lesions (“white spots”) in my brain, indicating active inflammation. My father referred me to a neurologist who performed a lumbar puncture (“spinal tap“) to confirm the MS diagnosis. I also saw a neuro-ophthalmologist who diagnosed me with optic neuritis – a common symptom of MS and the source of my eye pain and blurry vision.
Once diagnosed – similar to Selma Blair – I felt validated, almost relieved. My symptoms—the fatigue, headaches, vision problems, and sensory disturbances—were real, and I could now move forward with treating them.
Final Thought
While my MS journey began with a rocky start and would entail many more uphill battles, I can look back fifteen years later and see how living with MS has helped hone my role as a mother and physician. I’m more patient and resilient, a better listener, and can understand more deeply the invisible suffering of those living with a chronic illness.
In the end, learning to live fully and happily with MS has given me the strength to endure additional obstacles in life—and for that, I am grateful.
Who is the author?
Colleen Doherty, MD, is a board-certified internist and Verywell medical writer based in Chicago, Illinois. Colleen also has multiple sclerosis. She understands well the difficulty of balancing the demands and unpredictability of a chronic illness with a career and family.



![women [longevity live]](https://longevitylive.com/wp-content/uploads/2020/01/photo-of-women-walking-down-the-street-1116984-100x100.jpg)













