One aspect of wound care that does not receive as much attention as others is the long-term mental health impact that chronic or acute wounds have on patients. The importance of body image for well-being has recently begun to receive more attention in the age of social media, especially in terms of how it affects our mental health.
Chronic and acute wounds, particularly those that are disfiguring, that involve the face, or cause pain over long periods, tend to present significant challenges to both healthcare professionals and their patients. Not only are physicians treating them physically, but they’re also helping patients to cope with the impact of chronic and non-healing wounds on their mental health.
While helping patients to recover physically from an injury is always the primary objective, the psychological factor can have an effect on this as well. Patients with a positive attitude towards treatment can recover at significantly faster rates than those who do not.
And for those whose wounds are not expected to heal at all, wound care experts should be especially diligent. They should offer a hopeful future to those in long-term care. This is both one of the most rewarding and one of the most difficult endeavors in wound care today.
The Impact of Chronic and Acute Wounds on Mental Health
Studies have suggested that 12% of patients who make a full recovery from a critical injury continue to have psychological fallout from it even after one year, and as many as 58% are not able to work as much as they had prior to their injury. Nevertheless, little research has been conducted into how to help patients cope with the adjustment. This is most likely because psychological issues are much more difficult to identify and treat than physical ones. It may also mean that wound specialists may lack the language and training to articulate the problem.
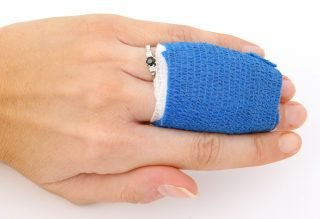
Image by Shutterbug75 from Pixabay
Part of the issue for chronic and acute wound patients is a lack of willingness to confront the reality of their situations. The human mind has a powerful ability to block out, distort, or ignore facts that make a person uncomfortable or disturb his or her self-perception.
For example, if a wound negatively affects the ability of the patient to do things physically that he or she had done before, he or she may end up in a state of denial, believing that everything is, in fact, the same as before. This can lead to frustration both for the patient and his or her family and friends.
In other cases, a patient may respond to his or her new reality by becoming withdrawn or depressed. They may even lose self-esteem or experience anxiety about the future. Grieving is also commonplace. If a patient’s care also involves a long stay in a health facility and/or a prolonged series of treatments, this can also place a heavy burden on his or her ability to endure the new reality.
A Caregiver’s Role in a Patients Mental Health

Caregivers can help patients to overcome these psychological traps by expressing acceptance, empathy, and warmth for them. Patients always respond positively when their caregiver expresses genuine interest in their well-being. They should also encourage the patient’s friends and family to remain empathetic and encouraging about the situation.
They should also encourage them to help him or her work through the process by focusing on the positive. Negative reactions from loved ones to chronic or acute injuries can have a devastating impact on a patient’s mental well-being. On the other hand, the opposite can be just as beneficial to the healing process.
Patient Self-Blame
In some cases, patients may also develop a sense of guilt or self-blame for their injury. Caregivers can help with this by encouraging patients to express their thoughts. They should try to help them understand the reality of their situation and the irrationality of their sense of responsibility. Moreover, they should always try to instill a sense of hope in patients based on the facts, but without resorting to building up false expectations.
The Importance of Social Support Networks
There are many other ways in which social bonding can help patients with chronic or acute wounds to cope, including involvement in social support networks, help from one’s religious community, or by pursuing interests and hobbies.

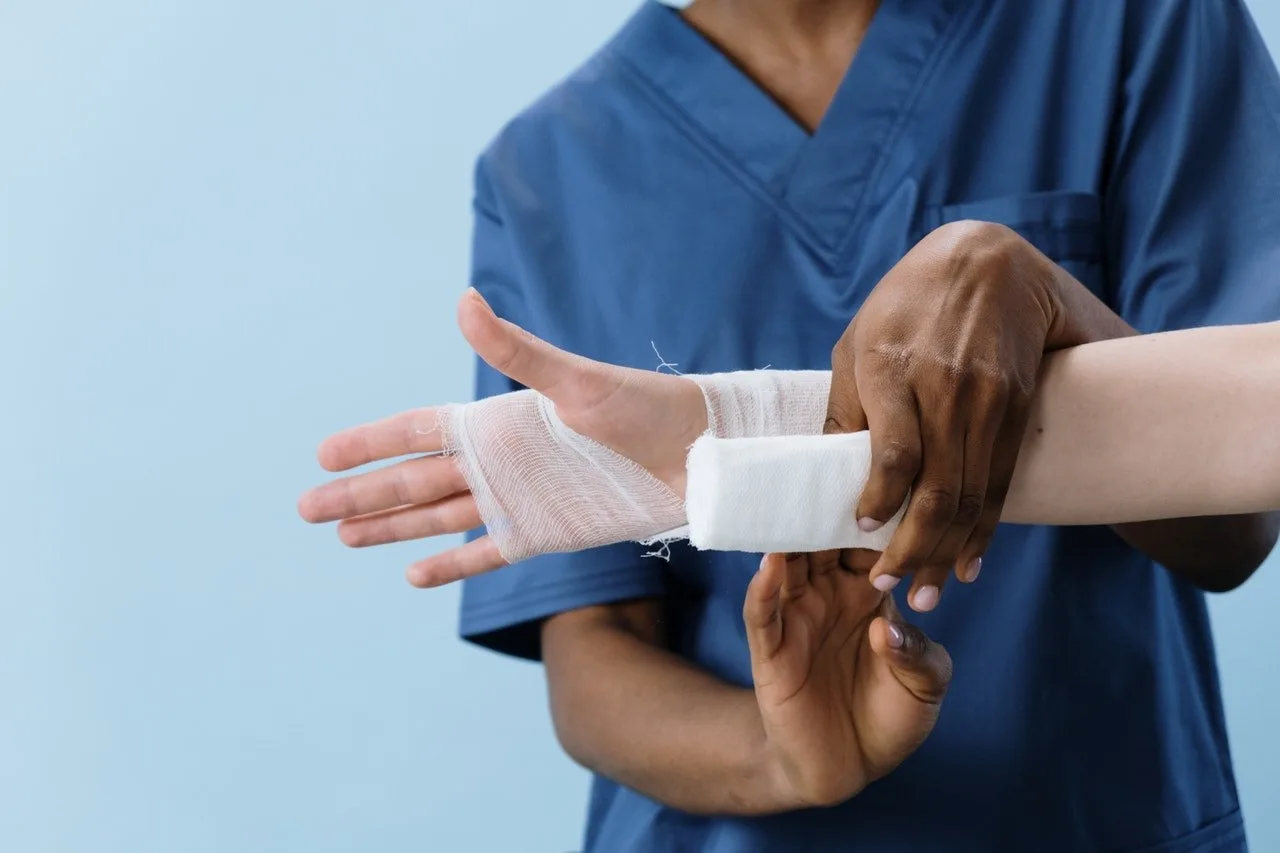
Photo by JESHOOTS.COM on Unsplash
Healthcare professionals can also help. They can do so by making the patient feel like a participant in his or her own treatment. They should keep them well-informed about every stage of the healing process. Healthcare professionals should also make them feel as if they are involved and empowered in it.
Helping the patient understand the facts about his or her wound can also go a long way toward helping them to properly cope with the circumstances and dispel uncertainties. After all, these uncertainties can lead to irrational fears if unaddressed. If the caregiver feels that a patient’s psychological state has gone beyond his or her ability to treat it, the patient should be given a referral to an appropriate specialist for further treatment.
Wound Patients in Psychological Distress
Numerous studies have already indicated that poor psychological health has a demonstrably negative impact on the body’s ability to heal. The length of recovery time from wounds can be significantly increased when a patient is in a poor mental state. This is because it can disrupt the immune system’s normal operation. Mental stress can also lead to the development of negative habits in patients, including smoking, drinking alcohol, and poor nutrition.
Some studies have also highlighted the risk that stress poses to a patient’s normal sleep patterns. This, in turn, can lead to a reduction in the body’s natural growth hormones. It can also slow down the body’s ability to repair damaged tissues. In this way, the intangibles of human psychology can have a very tangible effect on a patient when his or her needs are not properly addressed.
Physicians and Nurses Committment to Addressing Mental Health
Every medical practice should remain committed to addressing the mental well-being of its wound patients. Those who suffer from a chronic or acute wound, or those who know someone who does, know that it can be a challenging journey. But with the right support network, expertise, and ongoing wound care, patients can learn to take comfort in the healing process. They can also better accept whatever the reality of the situation has to offer.

Who is the author?
Gayle Morris is a freelance writer that’s been writing on health and wellness for over ten years. She spent over 20 years as a certified nurse and nurse practitioner. She then hung up her stethoscope and picked up the pen.
As a nurse, Gayle cared for patients at Cincinnati Children’s Hospital, Riley Children’s Hospital, Chicago Children’s Hospital (now Lurie Children’s Hospital), and at Methodist Hospital in Indianapolis. As a PNP, she worked at Mary Free Bed Rehabilitation Hospital in Grand Rapids, MI.
Health and wellness is Gayle’s passion and she loves boiling down complicated research studies into actionable strategies that help improve health.


![women [longevity live]](https://longevitylive.com/wp-content/uploads/2020/01/photo-of-women-walking-down-the-street-1116984-100x100.jpg)














Right on point.