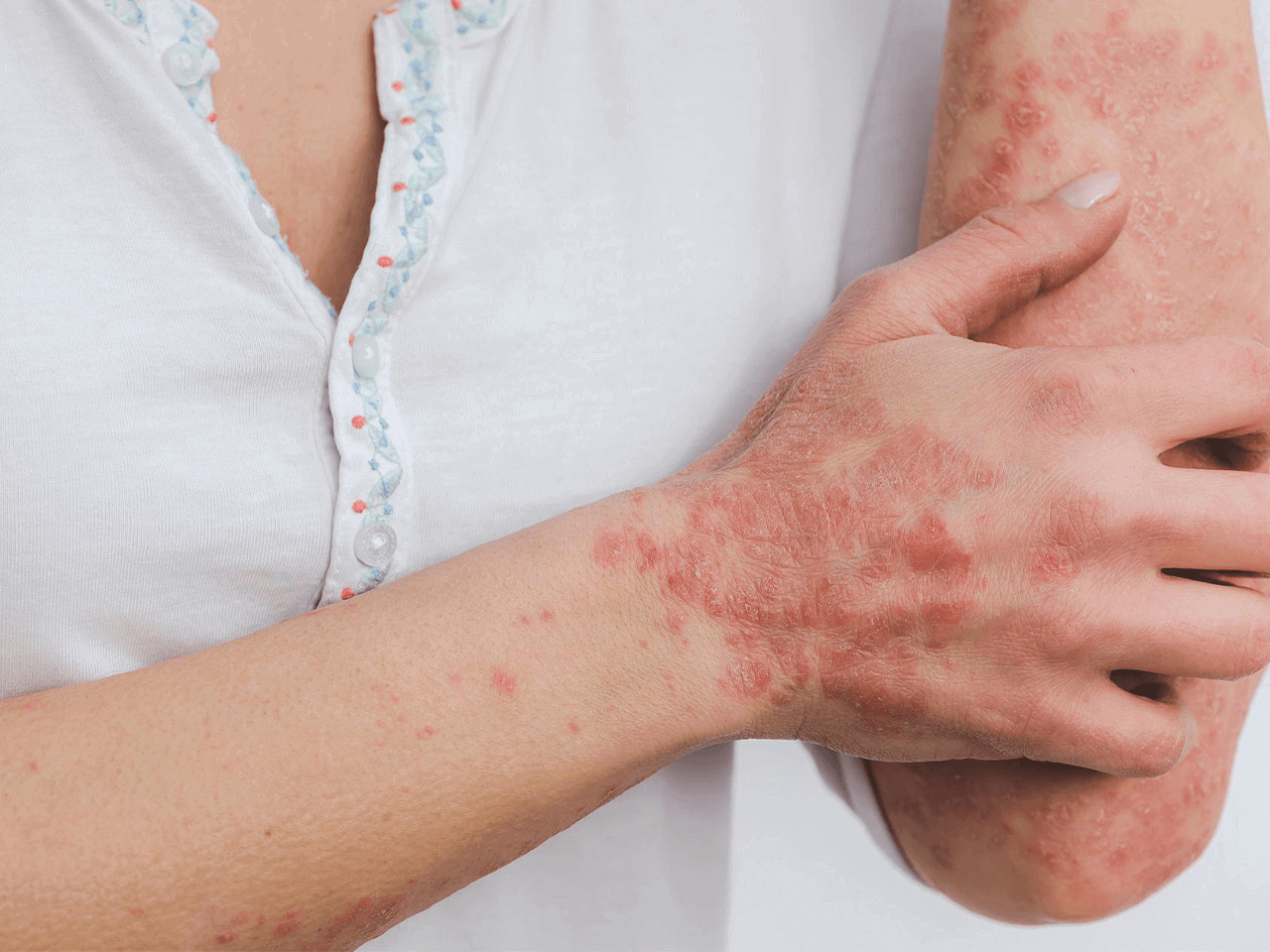
Psoriasis is a common, life-long, inflammatory skin condition which affects approximately 2% of the world’s population. In psoriasis, an overactive immune system speeds up the life cycle of the skin cells. Normally, healthy skin cells mature and shed from the skin’s surface every 28 days. In psoriasis, these cells reproduce much more quickly, usually within three to four days, and pile up on the skin surface. This causes the development of thick, scaly, red patches of skin. In this article dermatologist Dr. Tarryn Jacobs explains how to treat psoriasis.
The root causes of psoriasis begin inside the body, making it #MoreThanSkinDeep as the inflammation can impact other organs in the body. Diseases associated with psoriasis include psoriatic arthritis, diabetes, high blood pressure, and heart disease amongst others. Considering the above, seeing a dermatologist timeously is advised, as they can provide effective medical treatment.
How to treat psoriasis
To treat psoriasis the focus is centred around anti-inflammatory prescription medication. Depending on the severity of the condition, prescriptions include topical creams, light therapy, oral, and injectable medications.
How psoriasis affects the skin barrier
Psoriasis affects the skin’s hydration and the function of the skin barrier. The skin barrier is made up of multiple layers of cells called corneocytes, which can be considered as the “bricks” of a protective wall. They are held together by “glue”, which are the lipids in our skin, such as ceramides.
A healthy skin barrier maintains the water balance in the skin and protects against environmental aggressors such as UV rays, microorganisms, and pollution.
Two skincare tips
The fact that psoriasis affects the skin barrier means that good basic skin care practices are essential in conjunction with medical treatment. This can help to relieve dryness, itchiness, and strengthen the skin barrier function, which can improve the overall quality of life.
-
Cleanse your skin gently
It’s important to use gentle pH-balanced cleansers which can protect from further disruption of the fragile skin barrier.
-
Choose the ideal moisturiser
Moisturisers can help to reduce the dryness, scaling, and roughness of psoriasis-affected skin. A good moisturiser usually contains a combination of ingredients, namely emollients (e.g. dimethicone), humectants (e.g. glycerine) and occlusives (e.g. petroleum jelly). Ceramides are useful to seek out as they form the predominant component of the skin barrier and offer excellent barrier repair activity.
What active ingredients to look for in skin care products
Alongside moisturisers, there are several products containing active ingredients that can provide additional skin conditioning benefits in psoriasis.
Keratolytics, such as salicylic acid and urea, help promote the skin cell shedding process and can reduce the scaling of psoriasis-affected skin. Studies show that salicylic acid at 2-10% applied directly to psoriatic plaques can aid in softening them. Products containing 5% urea help to increase skin hydration and medication penetration.
Niacinamide, also known as vitamin B3, has anti-inflammatory properties and supports the skin barrier function by facilitating the formation of ceramides.
Coal tar has historically been used for approximately a century in the treatment of psoriasis, but its use has decreased over time, due to its odour and potential to cause irritation. Tar formulations can be found in numerous products from lotions to shampoos.

MaleWitch/Shutterstock
Can sun exposure make it better or worse?
Psoriasis can respond beneficially to UV radiation from natural sunlight or artificial sources (phototherapy). However, sun-induced aggravation of psoriasis can occur in around five to 24% of people, particularly in light skinned individuals. Sunburn can also provoke new areas of the condition in a process called a Koebner response. Daily sun protection is recommended with sunscreen of a minimum SPF of 30 to treat psoriasis.
Resources
Integrating a basic skin care approach improves the management of psoriasis flares ups and its remission phases. It is important to treat psoriasis early. Work with a dermatologist to determine which medication options will be best for you, but simultaneously taking good care of your skin may alleviate some of the discomforts that psoriasis can cause.
You can also join the #MoreThanSkinDeep Facebook Community, connect with people living with psoriasis who understand what you’re going through, and access valuable information and insights as you navigate your life with psoriasis.
References
1.Luger T, Seite S, Humbert P, Krutmann J, Triller R, Dréno B. Recommendations for adjunctive basic skin care in patients with psoriasis. Eur J Dermatol. 2014 Mar-Apr;24(2):194-200. doi: 10.1684/ejd.2014.2294. PMID: 24721699.
- Mijaljica D, Spada F, Harrison I. P. Topical Moisturisers for the Management of Psoriasis Vulgaris. In: Aghaei, A. P. S. , editor. Psoriasis [Working Title] [Internet]. London: IntechOpen; 2022 [cited 2022 Jun 26]. Available from: https://www.intechopen.com/online-first/80041 doi: 10.5772/intechopen.101964
- Passeron T, Lim HW, Goh CL, Kang HY, Ly F, Morita A, Ocampo Candiani J, Puig S, Schalka S, Wei L, Dréno B, Krutmann J. Photoprotection according to skin phototype and dermatoses: practical recommendations from an expert panel. J Eur Acad Dermatol Venereol. 2021 Jul;35(7):1460-1469. doi: 10.1111/jdv.17242. Epub 2021 May 4. PMID: 33764577; PMCID: PMC8252523.


![women [longevity live]](https://longevitylive.com/wp-content/uploads/2020/01/photo-of-women-walking-down-the-street-1116984-100x100.jpg)













